What Is Glaucoma? A Clear Explanation
Glaucoma is a term many people first hear during a routine eye examination — often before they have noticed any change in their vision.
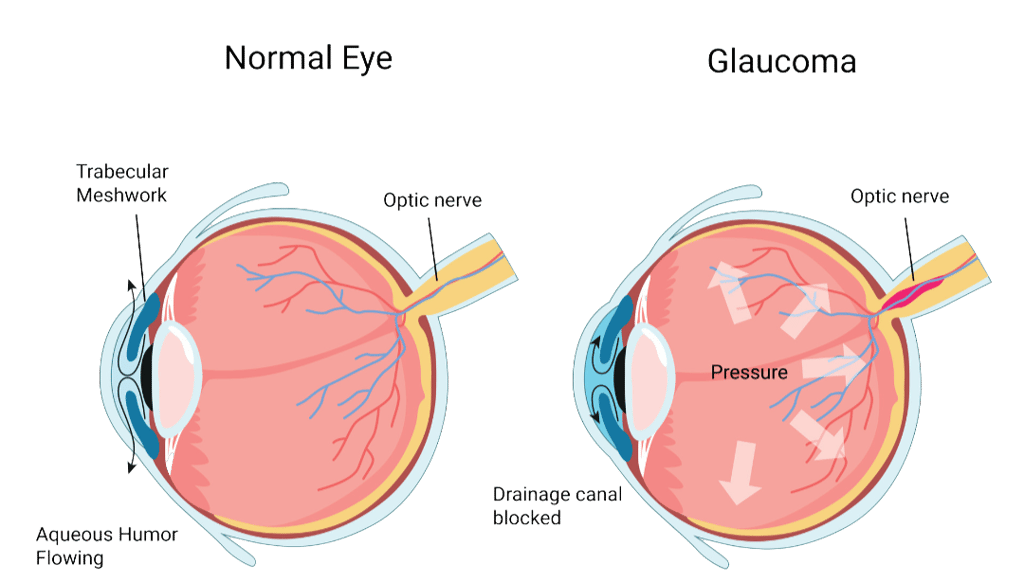
It refers to a group of eye conditions that damage the optic nerve, the structure that carries visual information from the eye to the brain. When this nerve is affected over time, vision can gradually change.
Understanding what is happening inside the eye can make the diagnosis feel far less confusing.
What happens in glaucoma?
The optic nerve is made up of more than a million tiny nerve fibers. These fibers transmit signals that allow you to see. In the most common type, primary open-angle glaucoma, some of these nerve fibers are slowly lost over time. This process is usually painless and develops gradually. As nerve fibers are lost, subtle changes begin to appear in the visual field, typically affecting side (peripheral) vision first. Central vision often remains normal in early stages.
Because these changes develop slowly, most people do not notice them at first. This is why glaucoma is often detected during routine testing rather than because of symptoms.
Are there different types of glaucoma?
Yes.
The most common form is primary open-angle glaucoma, which develops slowly over time and usually causes no early symptoms.
A less common form is angle-closure glaucoma. This occurs when the drainage angle inside the eye becomes blocked. In some cases, it can cause rapid eye pain, blurred vision, redness, headache, or nausea. Unlike open-angle glaucoma, acute angle-closure glaucoma requires urgent medical evaluation.
However, this form is much less common than the slow, open-angle type discussed above.
Why does eye pressure matter?
Inside the eye, a clear fluid is constantly produced and drained. This circulation maintains the eye’s shape and health. When the drainage system becomes less efficient, pressure inside the eye — called intraocular pressure (IOP) — can rise. Elevated pressure increases stress on the optic nerve.
However, pressure alone does not define glaucoma.
Some people develop optic nerve damage even when their eye pressure falls within what is considered a “normal” statistical range. Others may have elevated pressure without nerve damage (a condition known as ocular hypertension).
For this reason, glaucoma diagnosis is based on a combination of findings — not a single number.
How is glaucoma diagnosed?
There is no single test that confirms glaucoma on its own. Diagnosis is based on a structured evaluation that typically includes:
Careful examination of the optic nerve
OCT imaging to measure nerve fiber thickness
Visual field testing (perimetry) to detect blind spots
Measurement of intraocular pressure
Assessment of corneal thickness
These findings together help determine whether the optic nerve is being affected and whether progression is occurring.
What is the goal of treatment?
At present, damage to optic nerve fibers cannot be reversed. Treatment focuses on protecting the remaining vision. The primary strategy is lowering intraocular pressure to a level where further nerve damage is unlikely. This “target pressure” is individualized and may be adjusted over time.
Treatment may involve:
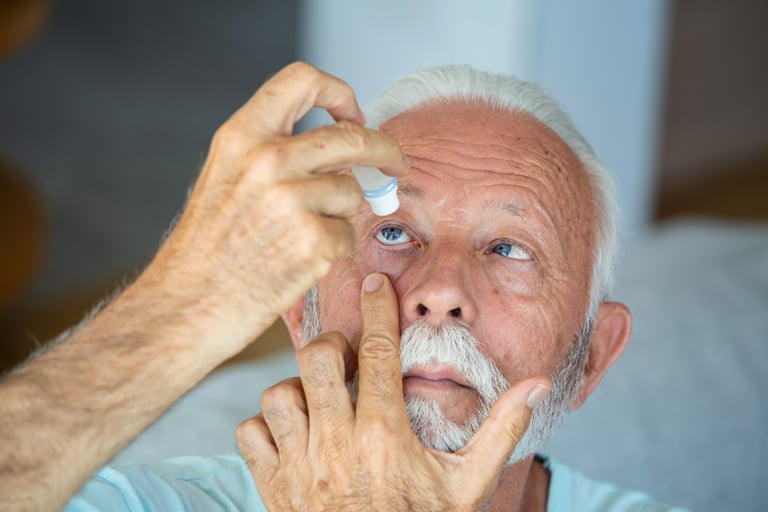
Prescription eye drops
Laser procedures to improve fluid drainage
Surgery in selected cases
Regular follow-up visits are essential. Glaucoma management is a long-term process focused on stability.
Will I go blind from glaucoma?
This is often the question people think about, even if they do not say it out loud. The honest answer is that most people with glaucoma do not go blind. When glaucoma is detected early and monitored regularly, treatment is effective at slowing or stopping further damage. Vision that has already been lost cannot be restored, but progression can often be controlled. Severe vision loss is more likely when glaucoma is advanced at diagnosis or when follow-up and treatment are inconsistent.
The key factor is ongoing care. With modern management and regular monitoring, most patients maintain useful vision throughout their lives.
Who is at higher risk?
Certain factors are associated with increased glaucoma risk, including:
Older age
Family history of glaucoma
African or Hispanic ancestry
Thinner corneas
Diabetes or cardiovascular disease
Long-term steroid use
Even without symptoms, individuals with these risk factors benefit from regular comprehensive eye examinations.
What should you take away from this?
Glaucoma usually develops slowly.
It is not an emergency in most cases.
With early detection, consistent monitoring, and appropriate treatment, most people maintain functional vision throughout their lives.
Understanding the condition is the first step. Ongoing care is what protects vision over time.


Bernani - Clear Eye Guidance
© 2026. All rights reserved.
