How Diabetes Affects the Eyes: A Clear Explanation
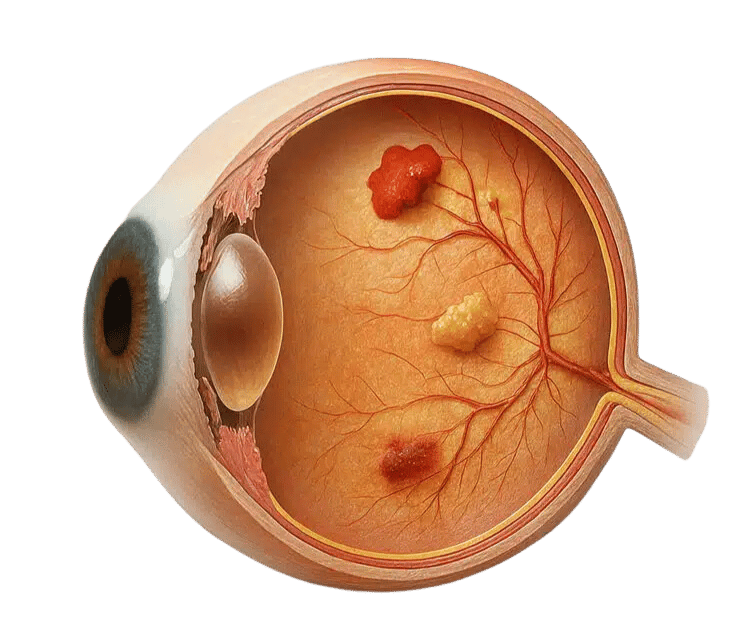
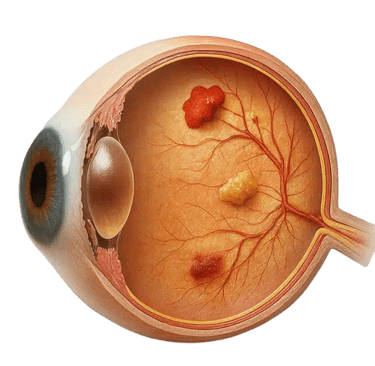
If you live with diabetes, you already know that blood sugar levels matter for your heart, kidneys, and nerves. They matter for your eyes, too. Diabetes affects the small blood vessels throughout the body. The retina — the light-sensitive tissue at the back of the eye — is especially dependent on healthy circulation.
Understanding what happens there makes the diagnosis much less mysterious.
What happens in the retina?
The retina contains tiny blood vessels that supply oxygen and nutrients. When blood sugar levels remain elevated over time, these vessels can become damaged. Their walls may weaken, leak fluid, or close off entirely. This process is called diabetic retinopathy.
In its early stages (non-proliferative diabetic retinopathy, NPDR), changes may include:
microaneurysms
small retinal hemorrhages
leakage causing swelling
Vision may still feel completely normal. In more advanced stages (proliferative diabetic retinopathy, PDR), the retina responds to poor circulation by forming new, fragile blood vessels. These vessels can bleed or cause scar tissue formation, which may lead to more serious complications.
What is diabetic macular edema?
The macula is the central part of the retina responsible for detailed vision — reading, driving, recognizing faces. If fluid leaks into this area, it can cause swelling known as diabetic macular edema (DME).
This may lead to:
blurred central vision
distortion
difficulty reading
Macular edema can occur at any stage of diabetic retinopathy.
Will I notice symptoms early?
Often, no.
One of the most important — and sometimes frustrating — aspects of diabetic eye disease is that early stages are usually silent. Vision may remain sharp even when retinal changes are already present.
That is why regular dilated eye examinations are essential, even when vision seems stable.
Can diabetes cause other eye problems?
Yes.
Diabetes is also associated with:
increased risk of cataracts
earlier onset of cataracts
higher risk of glaucoma
These are separate conditions, but their risk is elevated in people with long-standing diabetes.
Will I go blind?
This is a common concern. Most people with diabetes do not go blind. Severe vision loss is far less common today than it was decades ago, largely because of earlier detection and improved treatments.
The key factors are:
blood sugar control
blood pressure management
regular eye examinations
timely treatment when needed
When problems are detected early, modern therapies — including intravitreal injections, laser treatment, and surgery in selected cases — are highly effective at preserving vision.
How often should I have my eyes examined?
General guidance (consistent with AAO and ADA recommendations):
Type 1 diabetes: eye exam within 5 years of diagnosis
Type 2 diabetes: eye exam at the time of diagnosis
Pregnancy with diabetes: evaluation early in pregnancy
After that, examinations are typically recommended at least annually — sometimes more frequently depending on findings. Your eye doctor adjusts follow-up based on your individual situation.
What should you take away from this?
Diabetes can affect the eyes, but it usually does so gradually.
Early changes are often invisible without examination.
Most vision loss related to diabetes is preventable with consistent care.
Understanding the process is the first step. Regular follow-up is what protects your vision over time.
Bernani - Clear Eye Guidance
© 2026. All rights reserved.
